Surgery
Supporting Healing, Recovery, and Surgical Outcomes.
How HBOT Supports Surgical Recovery
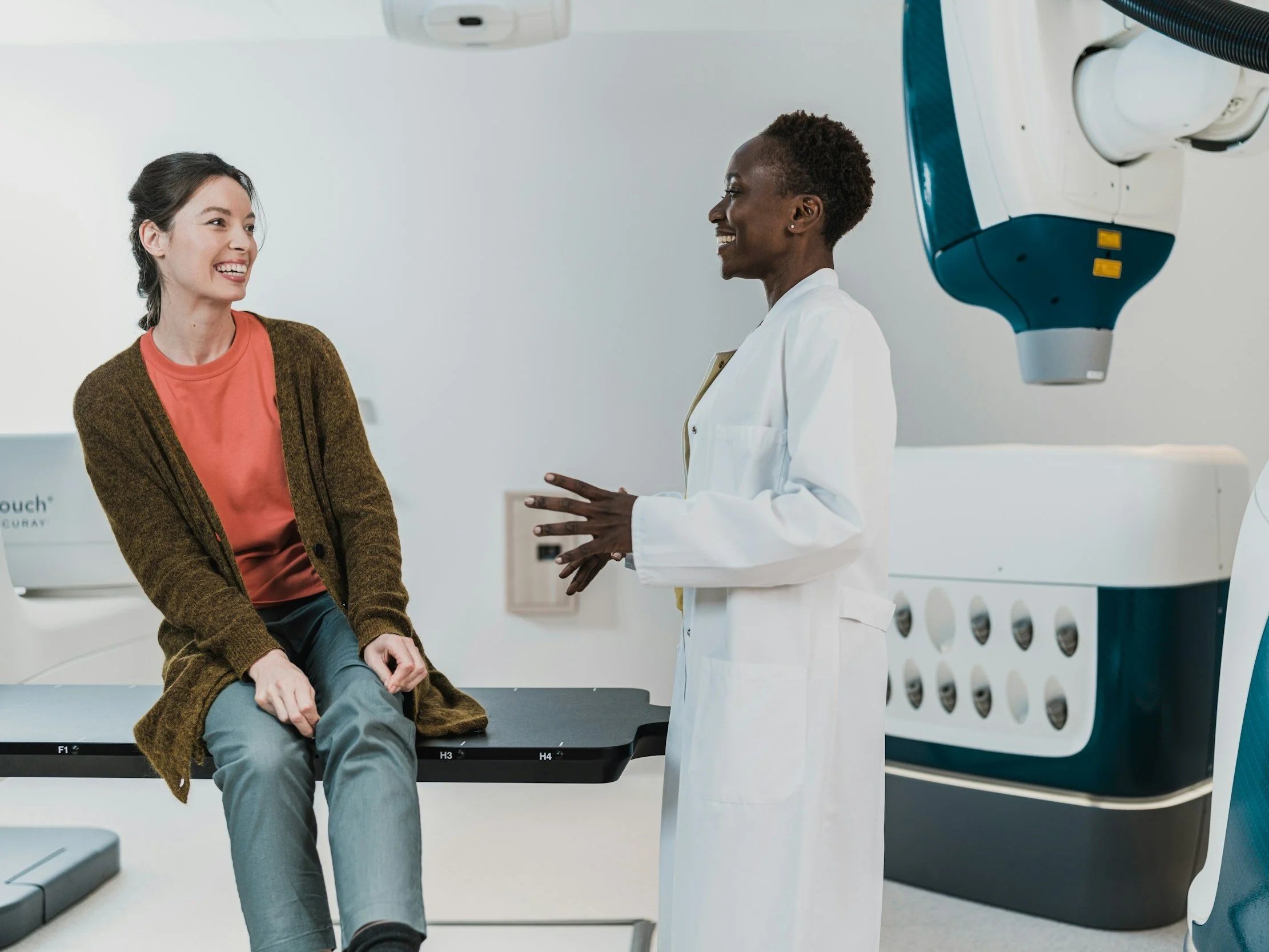
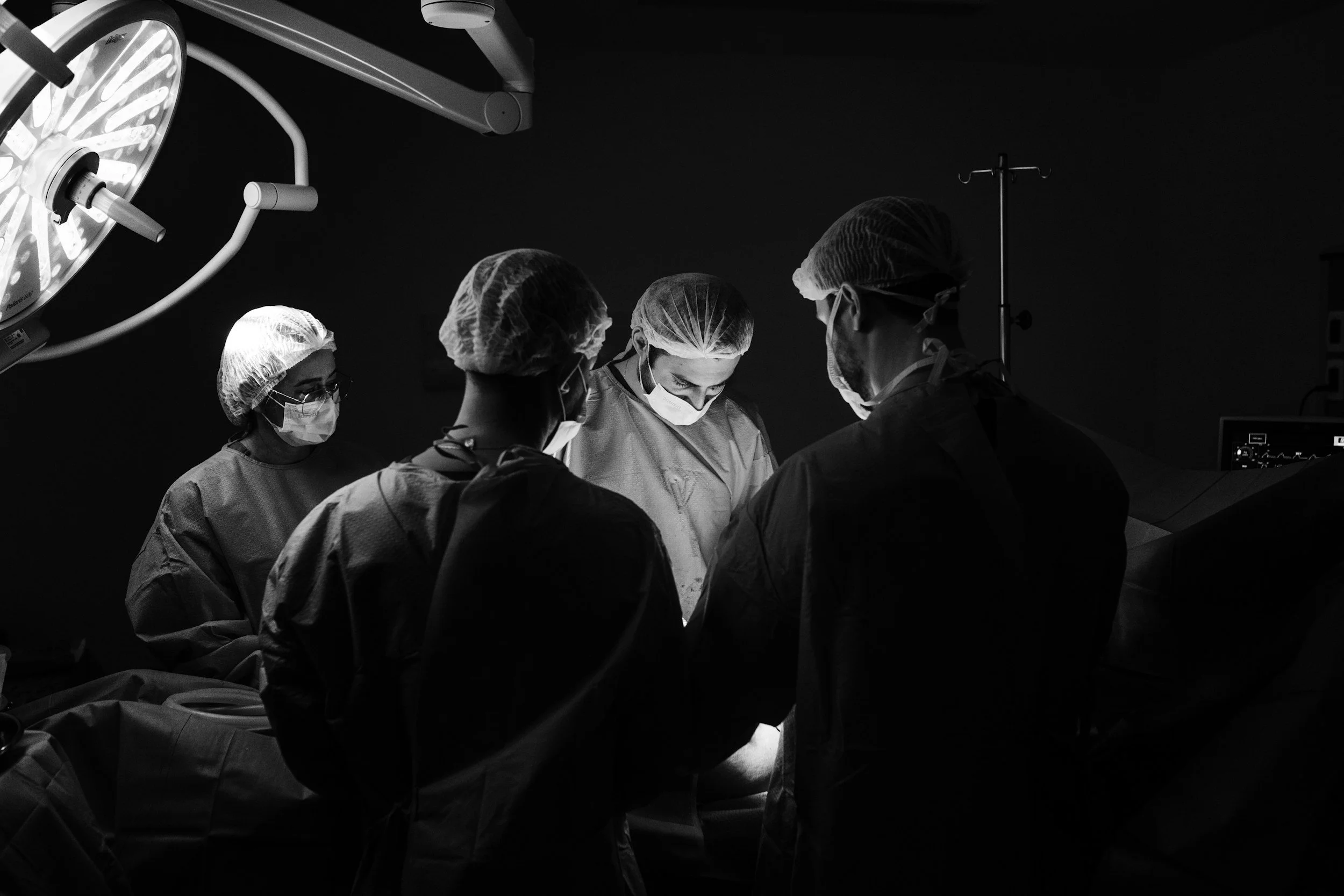
Surgery places significant stress on the body. From tissue trauma and inflammation to reduced oxygen delivery at the wound site, optimal recovery depends on how effectively the body can heal. Hyperbaric Oxygen Therapy (HBOT) is a clinically recognised adjunct therapy that supports faster, safer healing before and after surgery by enhancing oxygen delivery at a cellular level.
HBOT is used internationally in hospital and outpatient settings to support surgical recovery, particularly where healing may be compromised.
HBOT supports several key healing mechanisms:
Accelerated wound healing
Improved tissue repair and regeneration
Reduced post-operative inflammation and swelling
Enhanced immune response
Lower risk of infection
Improved outcomes in complex or slow-healing wounds
The result? Faster recovery times, lower infection risk, and reduced physical discomfort.

Key Recovery Benefits
-

Enhanced Wound Healing
Oxygen is essential for collagen formation, angiogenesis (new blood vessel growth), and epithelial repair. HBOT has been shown to significantly improve healing in surgical wounds, grafts, and flaps, particularly where blood supply is compromised.
-
Reduced Surgical Complications
Clinical studies demonstrate that HBOT can reduce the risk of:
- Wound breakdown
- Infection
- Tissue necrosis
- Delayed healing following major or reconstructive surgery
-

Improved Outcomes in High-Risk Patients
HBOT is especially beneficial for patients with factors that impair healing, including:
- Diabetes
- Vascular disease
- Previous radiation therapy
- Autoimmune or inflammatory conditions
- Repeat or revision surgeries
-
https://pubmed.ncbi.nlm.nih.gov/41018185/
A systematic review and meta-analysis of 11 randomized trials found that adding hyperbaric oxygen therapy (HBOT) to standard care after intracranial aneurysm surgery significantly enhanced neurological recovery, functional independence, and quality of life versus standard care alone.
-
https://pmc.ncbi.nlm.nih.gov/articles/PMC10145168/
A narrative review showed that HBOT can promote wound closure and epithelialization and has potential benefits in managing surgical site infections following procedures like cardiac or urogenital surgery via enhanced oxygen-mediated antimicrobial activity.
-
https://pubmed.ncbi.nlm.nih.gov/24343585/
Clinical trials on acute surgical and traumatic wounds (e.g., skin grafts and crush injuries) suggest HBOT may increase graft survival and reduce tissue necrosis compared to standard care, although larger, high-quality studies are still needed.
-
https://pubmed.ncbi.nlm.nih.gov/27041554/
Animal research on ischemic colorectal surgery found that HBOT prevented anastomotic breakdown and improved tissue integrity when applied before and after surgery, suggesting improved oxygenation benefits surgical healing.
What the research says.
Typical Surgery Protocols
Pre-surgical HBOT
3 - 5 sessions prior to surgery to help improve tissue oxygenation, circulation, and cellular readiness—particularly in areas with compromised blood flow or prior radiation exposure.
Post-surgical HBOT
5- 20 sessions, typically delivered as close together as possible. These sessions aim to support wound healing, reduce inflammation, assist in infection management, and promote recovery of stressed or healing tissues.
HBOT is always provided in coordination with the patient’s surgical and medical team and does not replace standard surgical care.

What our clients think…