How Many HBOT Sessions Do You Need for Surgery Recovery?
If you're preparing for surgery, or already in recovery, and you've been looking into hyperbaric oxygen therapy, the first question most people ask is a simple one: how many sessions will I actually need?
It's a reasonable question, and it doesn't have a single, universal answer. The honest response is: it depends on the type of surgery, the complexity of your recovery, and your individual health. But there are well-established protocols based on clinical research, and at OxyPlus, our HBOT clinic in Newcastle, we design personalised treatment plans around exactly these factors.
This post walks through what the research says, what the different session ranges mean in practice, and how to think about HBOT as part of your surgical recovery plan.
Why Surgery Creates an Oxygen Problem
All surgery, no matter how routine, creates a wound. And wound healing is fundamentally an oxygen-dependent process.
When tissue is cut, sutured, or grafted, local blood vessels are disrupted. The result is a period of relative hypoxia (low oxygen) in exactly the tissue that needs it most. This oxygen deficit slows every aspect of healing: collagen formation, new blood vessel growth, immune cell activity, and cellular repair.
HBOT directly addresses this problem. By breathing 100% pure oxygen at high atmospheric pressure, the amount of oxygen dissolved in blood plasma increases dramatically. Reaching tissues that compromised blood flow can't adequately supply. This accelerates the biological cascade of healing at precisely the right time.
The research is clear on how HBOT supports post-surgical healing. The more nuanced question is how much is needed, and that's where surgery type, complexity, and individual factors come in.
What HBOT Does During Surgical Recovery
Before looking at session numbers, it helps to understand what HBOT is actually doing during each session. Research has identified several distinct mechanisms relevant to post-surgical healing:
Angiogenesis — HBOT stimulates the release of vascular endothelial growth factor (VEGF) and other growth factors, triggering the formation of new blood vessels. This restored circulation is critical for long-term tissue recovery and is typically seen from around 10 sessions onward.
Collagen synthesis — Increased oxygen levels enhance fibroblast proliferation and activity. Fibroblasts are the cells responsible for producing collagen, the structural protein that gives healed tissue its strength. Collagen synthesis is oxygen-dependent, meaning HBOT directly accelerates this process.
Reduced swelling and oedema — HBOT causes mild vasoconstriction of healthy blood vessels, which paradoxically reduces post-operative swelling without compromising oxygen delivery to damaged tissue. Many clients notice a reduction in swelling and bruising within their first few sessions.
Infection resistance — Oxygen-rich tissue is significantly more resistant to bacterial growth, particularly from anaerobic bacteria. HBOT reduces post-operative infection risk, a clinically significant benefit given that surgical site infections are one of the most common post-operative complications.
Stem cell mobilisation — Research has shown that after 20 sessions of HBOT, there is an observed eight-fold increase in circulating stem cell markers, highlighting HBOT's potent role in mobilising the body's own repair cells for tissue regeneration.
Reduced inflammation — The anti-inflammatory response is notably rapid. Research documents significant reductions in inflammatory markers within just four days of beginning HBOT. For post-surgical inflammation that delays recovery, this is particularly meaningful.
Before Surgery: The Pre-Operative Case
One aspect of surgical HBOT that's less well-known is its use before the operation. Pre-operative HBOT optimises tissue oxygenation and healing potential in the days before surgery. Essentially topping up the tissue's oxygen reserves and priming the repair machinery before the wound is even made.
Research has shown that a single pre-operative HBOT session significantly reduced complication rates in complex surgeries including pancreaticoduodenectomy. For patients undergoing high-risk procedures or those with comorbidities, a short course of 3–5 sessions before surgery, followed by a post-operative course, may be appropriate.
At OxyPlus Newcastle, we discuss both pre- and post-operative options during your initial consultation, tailoring the approach to your specific procedure and health profile.
Does Surgery Type Change the Protocol?
Yes, significantly. Here's a quick guide to how different surgery types map to the session frameworks above:
Cosmetic and aesthetic surgery (rhinoplasty, facelift, breast augmentation, liposuction): Typically 5–10 sessions post-operatively for standard recovery; 10–20 for more extensive body contouring procedures.
Orthopaedic surgery (joint replacement, ACL reconstruction, spinal surgery): 10–20 sessions recommended, given the depth of tissue involved and the importance of collagen and angiogenesis for long-term joint and tendon recovery.
Reconstructive surgery following trauma or cancer: 20+ sessions, with individual assessment. Post-radiation tissue often requires longer courses.
Abdominal surgery (hernia repair, appendectomy, laparoscopic procedures): 5–10 sessions for uncomplicated cases.
Skin grafts and flap surgery: HBOT is particularly well-evidenced for graft survival. Skin grafts are in a state of hypoxia immediately post-surgery, and HBOT has been shown to improve graft viability through enhanced oxygenation, angiogenesis, and anti-infective effects.
Dental and oral surgery (including implants, jaw surgery, extractions following radiotherapy): 5–20 sessions depending on complexity. Osteoradionecrosis of the jaw, a known complication of radiotherapy, is one of the FDA-approved indications for HBOT.
What Happens Session by Session: A Timeline
Understanding when each effect kicks in helps clarify why session numbers matter, and why cutting a course short may not deliver the full benefit.
Sessions 1–5: Antioxidant and anti-inflammatory effects begin within 24 hours of the first session. By sessions 3–5, most patients notice a meaningful reduction in post-operative swelling and bruising. Cellular energy and tissue function begin to improve.
Sessions 5–10: Substantial pain relief is commonly reported. Wound closure accelerates. Early fibroblast activity and collagen production begins to increase measurably.
Sessions 10–20: Angiogenesis is actively promoted, new capillary beds form to restore circulation to healing tissue. Collagen density increases. Stem cell activity begins to rise significantly.
Sessions 20+: Eight-fold increase in circulating stem cell markers documented. Maximum tissue regeneration effects. Critical for patients with healing complications or underlying comorbidities.
Important Factors That Influence Your Session Number
Beyond surgery type, several individual factors meaningfully affect how many sessions are likely to be most beneficial:
Underlying health conditions — Diabetes, obesity, peripheral vascular disease, autoimmune conditions, and a history of smoking all impair healing and suggest a longer course.
Age — Tissue healing capacity declines with age. Older patients generally benefit from more sessions to achieve equivalent outcomes.
Timing — Starting HBOT early (ideally within 72 hours post-surgery) maximises the benefit. Delayed starts may require additional sessions to achieve comparable results.
Surgery complexity and site — Deeper wounds, areas with poor natural circulation, and surgeries involving bone or cartilage require more extensive tissue regeneration and therefore more sessions.
Response to treatment — Some patients respond faster than others. At OxyPlus, we monitor progress and adjust accordingly.
A Note on Expectations
HBOT is not a guarantee of complication-free surgery or perfect healing. It is a well-evidenced adjunct that improves the odds significantly, reducing healing time, lowering complication risk, and supporting better long-term tissue quality. The research is strong, and we're transparent about both what it can and cannot do.
We always recommend discussing HBOT with your surgeon before beginning treatment, and all OxyPlus clients undergo a thorough consultation before their first session. We can also liaise with your surgical team if helpful.
HBOT for Surgery Recovery in Newcastle — What to Expect at OxyPlus
At OxyPlus, Newcastle's specialist hyperbaric oxygen therapy clinic, we work with clients preparing for and recovering from a wide range of surgeries. We're conveniently located in Newcastle, making us accessible for patients across the North East including Gateshead, Sunderland, Durham, and Northumberland.
Here's how we approach post-surgical HBOT:
Initial Consultation — We discuss your surgery type, date, health history, and recovery goals, and design a personalised session plan.
Flexible Scheduling — We work around your recovery timeline, whether that means daily sessions in the immediate post-operative period or a longer spread-out course.
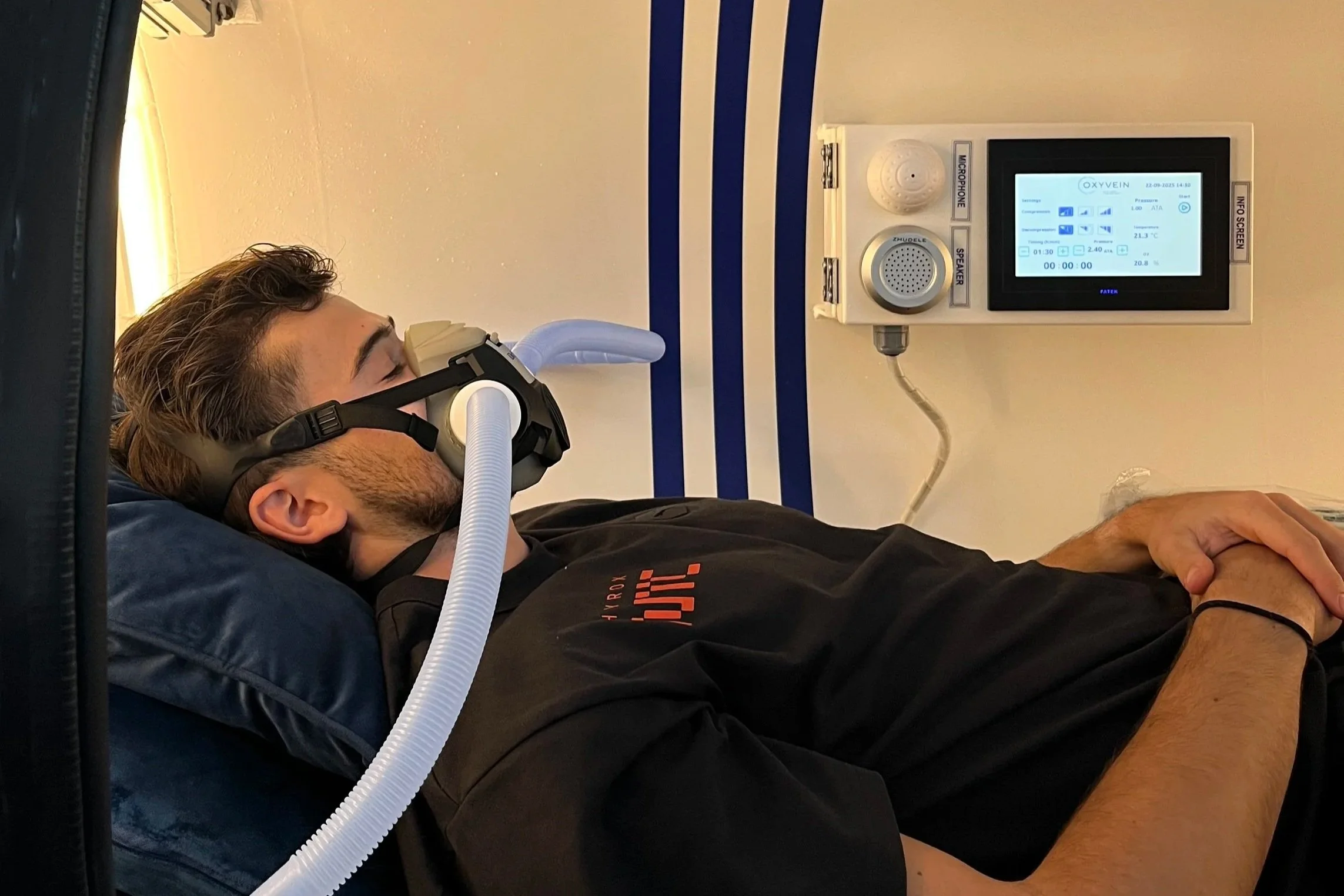
Medical-Grade Sessions — All sessions take place in our clinical hyperbaric chambers with 100% oxygen under atmospheric pressures of up to 2.4ATA. Sessions are supervised and typically 60–90 minutes.
Progress Review — We check in throughout your course and can adapt the plan based on how your recovery is progressing.
Frequently Asked Questions About HBOT and Surgery Recovery
Q: How soon after surgery can I start HBOT? A: Ideally within 24–72 hours of the procedure, provided your surgeon is happy. The earlier HBOT begins, the more it can influence the acute inflammatory and healing phase. Some clinics recommend starting the day after surgery for elective procedures.
Q: Can I have HBOT before surgery? A: Yes. Pre-operative HBOT is used to prime tissue oxygenation and healing potential before the wound is made. A short course of 3–5 sessions in the week before surgery, combined with post-operative treatment, can further improve outcomes, particularly for high-risk cases.
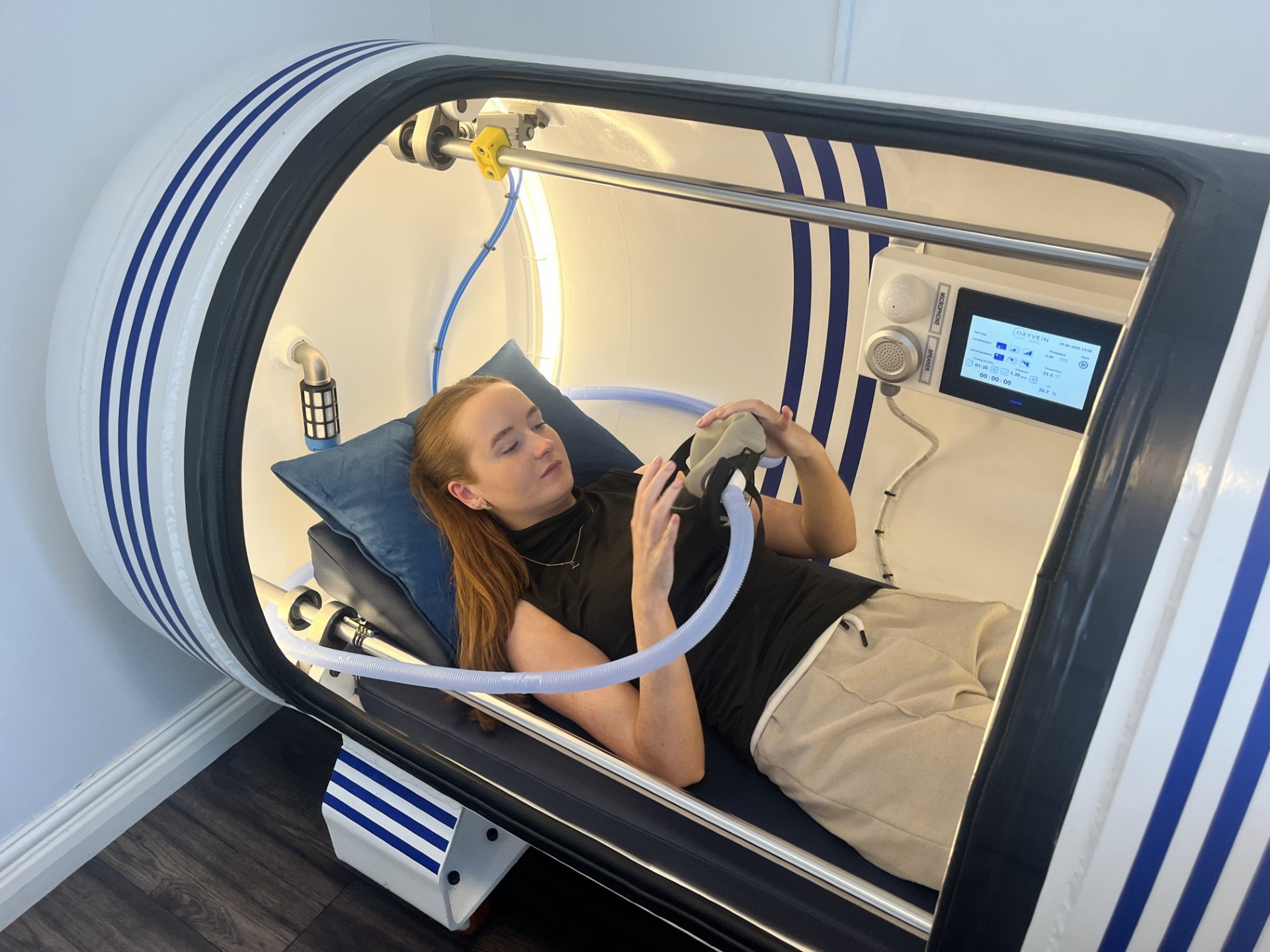
Q: How long is each HBOT session? A: At OxyPlus Newcastle, sessions are typically 60–90 minutes. You relax in the hyperbaric chamber breathing 100% oxygen, most clients find sessions comfortable and restful.
Q: Is HBOT safe after surgery? A: HBOT has a well-established safety profile. There are some contraindications, which is why we conduct a thorough health consultation before beginning treatment. We always recommend informing your surgeon you are undertaking HBOT as part of your recovery.
Q: Will my surgeon know about HBOT? A: Awareness varies. Some surgeons actively recommend it; others may be less familiar with the evidence. We can provide information to share with your surgical team, or liaise directly if helpful.
Q: How many HBOT sessions for knee replacement recovery? A: Based on the clinical research, including a 2025 randomised controlled trial in Scientific Reports, a course of 10–20 sessions is typically appropriate for knee replacement recovery, targeting both the early inflammatory phase and the deeper tissue regeneration phase.
Q: Where can I get HBOT for surgery recovery in Newcastle? A: OxyPlus is Newcastle's specialist HBOT clinic, offering medical-grade hyperbaric oxygen therapy with a thorough clinical consultation process. Visit oxyplus.co.uk to book your consultation or speak to us about timing around your procedure.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult your surgeon or a qualified healthcare professional before beginning HBOT as part of your surgical recovery. Individual results vary.